Contents
- 1 Androgenetic Alopecia (Male Pattern Baldness)
- 2 Autograft
- 3 Allograft
- 4 Bulge Area
- 5 Camouflage
- 6 Club Hair (Telogen hair)
- 7 Companion Layer
- 8 Dermal Papilla
- 9 Dissection
- 10 Donor Area
- 11 Donor Density
- 12 Donor Dominance
- 13 Finasteride/Dutasteride
- 14 Follicle
- 15 Follicular Unit
- 16 Follicular Unit Dissection
- 17 Follicular Unit Graft
- 18 Follicular Unit Extraction (FUE)
- 19 Follicular Unit Transplantation (FUT)
- 20 Follicular Unit Hair Transplantation (FUHT)
- 21 Follicular Pairing
- 22 Front of Scalp
- 23 Graft Excision
- 24 Grafts Cut to Size
- 25 Hair Shaft
- 26 Lateral Slits (Coronal Slits, Horizontal Slits)
- 27 Mid-scalp (Top)
- 28 Miniaturization
- 29 Micro-graft
- 30 Mini-graft
- 31 Mini-Micrografting
- 32 Norwood Classification
- 33 Post-Hair Transplant Effluvium
- 34 Recipient Area
- 35 Recipient Site
- 36 Senile Alopecia
- 37 Sagittal Slits (Vertical slits)
- 38 Sebum
- 39 Theory of Donor Dominance
- 40 Vasoconstrictor
- 41 Vellus Hair
- 42 Vertex (Crown)
- 43 Vertex Transition Point (VTP)
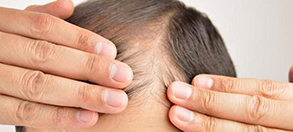
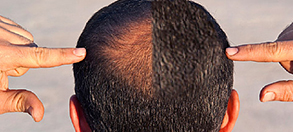
Androgenetic Alopecia (Male Pattern Baldness)
The most common type of hair loss in men. It is caused by the genetic susceptibility of hair follicles to the hormone DHT. It affects the central and frontal area of the scalp and the crown. It may eventuate in a U-shape configuration of hair loss.
Autograft
A graftn is taken from one part of the body and moved to another. In a hair transplant, the follicular unit grafts are autografts.
Allograft
A graft is taken from one person and grafted to another (i.e. kidney transplant). Immunosuppressive agents must be used with allograft transplants so that the grafts are not rejected by the host.
Bulge Area
The central region of the hair shaft that divides the permanent section of the hair (infundibulum and isthmus) from the lower non-permanent region (suprabulbar and bulbar) and is marked by the attachment of the arrector pili muscle. It is thought that the bulge area contains the stem cells that help regenerate the hair shaft. The bulge area like the upper hair shaft is also considered a permanent part of the hair shaft.
Camouflage
Camouflage in hair restoration repair involves the placement of small grafts (micrografts or follicular units) in front of larger ones to make them look more natural.
Club Hair (Telogen hair)
A hair that has stopped growing. One that is in the telogen (resting) phase of the hair cycle. It is anchored to the skin with its “club-like” root, but will eventually be pushed out and replaced by a new growing hair.
Companion Layer
In between the outer root sheath (ORS) and the inner root sheath (IRS) of the hair follicle lies the companion layer, which is a single layer of flattened cells. The companion layer acts a slippage plane to allow the IRS-sheathed hair shaft to move up in conjunction with Henle’s layer while the ORS remains stationery.
Dermal Papilla
The dermal papilla is situated at the base of the hair follicle. The dermal papilla is composed of fibroblasts, blood vessels, and nerves. This structure is extremely important in the regulation of hair growth and is a key element in hair cloning, as the cells that make up the dermal papilla (fibroblasts) can be multiplied.
Dissection
To separate tissue so that the internal structure can be examined and its function and relationship of its components discerned. In follicular unit hair transplantation, it refers to the isolation of follicular unit grafts from a donor strip using a stereo-microscope.
Donor Area
The donor area, also known as the safe donor area, is the region in the back of the scalp (occipital scalp) that remains throughout one’s lifetime even in the setting of advanced male pattern baldness or androgenetic alopecia . This horseshoe shaped area is harvested during a hair transplant by strip harvesting and transplanted into the recipient area. What was discovered in the 1950s was that this occipital hair genetically programmed would not be lost when moved into bald areas of the scalp through a condition known as donor dominance.
Donor Density
The number of hair in the donor area measured per square centimeter. The higher number of hairs per square centimeter, i.e., the greater the donor density, the more “paint”, i.e., hairs, that can be used to paint the “canvas”i.e., the bald scalp. An individual with high donor density can have a much higher chance of filling a wide area of baldness than someone with medium or low hair density. Donor density ranges in general between 60 to 120 follicular units per square centimeter.
Donor Dominance
The phenomenon discovered by the famed New York Dermatologist, Norman Orentriech, in the 1950s that when hair was transplanted from the back of the head into the balding frontal region would continue to grow and not be lost, i.e., the transplanted hair would maintain the characteristic of the donor site and not be influenced by the recipient site. This is the principle of modern hair restoration but is not entirely true as the recipient site can have some influence.
Finasteride/Dutasteride
The generic form of the brand-name drugs Propecia and Proscar. Propecia is the 1mg tablet of finasteride used for the treatment of hair loss. Finasteride works to prevent hair loss by blocking the formation of dihydrotestosterone (DHT) by inhibiting the enzyme 5 alpha-reductase. Proscar is manufactured by Merck and is FDA approved for the treatment of benign prostate enlargement.
Follicle
The structure in the scalp that produces a hair.
Follicular Unit
Hair follicles that grow together naturally as a group. They share the same blood supply, nerves and muscle (arrector pilorum). The follicular unit of the adult human scalp consists of 1-4, and occasionally 5, terminal hair follicles, 1, or rarely 2, vellus follicles and is surrounded by a band of collagen. In a follicular unit hair transplant, only intact follicular units are used in the procedure.
Follicular Unit Dissection
A hair transplant technique in which naturally occurring, individual follicular units are dissected intact from a strip of donor tissue that is removed during the hair transplant procedure. The technique involves the use of a dissecting stereo-microscope of at least 6-10x magnification to isolate the follicular unit grafts.
Follicular Unit Graft
A graft that is comprised of a single, intact follicular unit of 1-4 hairs. It is the only type of graft that is used in follicular unit hair transplant procedures.
Follicular Unit Extraction (FUE)
A procedure where individual follicular units are removed directly from the donor area. Because this hair restoration procedure often does not produce completely intact follicular units, this procedure may not be considered follicular unit transplantation in the strictest sense.
Follicular Unit Transplantation (FUT)
A method of hair restoration surgery where hair is transplanted exclusively in its naturally occurring, individual follicular units. Single strip harvesting and stereomicroscopic dissection are required in the standard definition of this hair transplant procedure. More recently, follicular unit extraction techniques are also considered a subset of this procedure.
Follicular Unit Hair Transplantation (FUHT)
FUHT is just the more wordy version of FUT. It describes the same procedure. Since a follicle is “hair,” the word hair in the title is redundant.
Follicular Pairing
Placing two follicular unit grafts (FUG, See Follicular Unit Graft) into one recipient site to create a larger single graft in an area like the central scalp that would benefit from larger sized grafts when there is an insufficient number of these larger sized follicular units.
Front of Scalp
In surgical hair restoration, this term refers to the frontal portion of the scalp that includes the frontal hairline and the area immediately behind it. In a hair transplant, the greatest density is often placed in this region of the scalp. In an average person, the frontal area measures approximately 30-50 cm2.
Graft Excision
Graft excision is a hair transplant repair technique where large or improperly positioned grafts are excised (removed). The large graft is usually divided up into smaller units and then re-implanted in a more natural distribution and direction. Graft excisions are usually performed prior to camouflage techniques in hair transplant repair.
Grafts Cut to Size
A dissection technique used in hair transplants where the donor strip is subdivided to produce grafts of specific sizes defined by the number of hairs they contain and/or the size of tissue that will fit into a specific recipient site. The dissection is usually performed without microscopic control.
Hair Shaft
The dead portion of the hair that protrudes from the surface of the skin. It is made predominantly of the protein keratin.
Lateral Slits (Coronal Slits, Horizontal Slits)
A specific orientation of recipient sites made so that the length of the slit lies parallel to the hairline. This hair transplant technique is felt to offer better coverage than other recipient site orientations, as the hair from the grafts placed in lateral slits tends to fan out over the scalp.
Mid-scalp (Top)
The area on the top of the head between the front and the vertex (crown). Hair on the mid-scalp points in a predominantly forward direction.
Miniaturization
The progressive decrease in hair shaft diameter and length due to the actions of DHT on the hair follicle. Miniaturization is the key change seen in androgenetic alopecia. Densitometry is used to identify miniaturization in its early stages. When evaluating a person for hair restoration surgery, it is important to assess the degree of miniaturization in the back and sides of the scalp to be certain that the donor area is permanent.
Micro-graft
Technically, a 1-2 hair graft. It does not necessarily need to be a follicular unit but may be two 1-hair units or part of a 3-hair unit etc. The term micro-graft is used more generally in hair transplant surgery as any small graft.
Mini-graft
Technically, a 3-6 hair graft derived from either a single follicular unit, multiple follicular units, or multiple, partial follicular units. In practice, hair transplant surgeons often call grafts containing up to 10 or more hairs mini-grafts.
Mini-Micrografting
A method of hair restoration surgery which uses grafts containing 1-6 hairs, in groups that do not necessarily correspond to the naturally occurring follicular units. In this type of hair transplant procedure, the micro-grafts are generally placed at the frontal hairline and the mini-grafts behind them (for density). Mini-micrografting procedures, although technically easier to perform, do not look as natural as follicular unit transplantation.
Norwood Classification
A scale for the classification of hair loss developed by O’tar Norwood in 1975. It was based upon an earlier classification of Hamilton. The Norwood scale is used by hair transplant surgeons to describe the extent of a person’s hair loss. The regular class has 7 stages and the A class has five.
Post-Hair Transplant Effluvium
Also referred to as shock loss, is shedding of some of the patient’s existing hair in the area of the transplanted hair following a hair transplant procedure. The term does not refer to the shedding of the transplanted hair – which is almost universal. The shedding generally begins a few weeks after the hair transplant and can persist for three or four months.
The condition is often reversible, although hair that is at the end of its life span (i.e. miniaturized) may not return. Propecia (Finasteride) may be protective of this to some degree. Post-transplant effluvium can be more significant in women than in men, since when performing surgical hair restoration in women, hair is commonly transplanted into to areas of thinning (with existing miniaturized hair).
Recipient Area
The region on the balding scalp that hair is transplanted into during a hair restoration procedure.
Recipient Site
A tiny hole or slit made in the recipient area by a needle or other sharp instrument to accommodate a graft during a hair transplantation procedure.
Senile Alopecia
A type of hair loss that naturally occurs with age. During the process of aging, both the duration of hair growth and the diameter of the hair follicle decrease, producing finer and shorter hairs. The process occurs over the entire scalp and tends to be more uniform than the changes of miniaturization associated with the effects of DHT. The exact mechanism of senile hair loss is unclear.
Sagittal Slits (Vertical slits)
The traditional method of orienting recipient sites in a hair transplant where the length of the slit lies perpendicular to the hairline.
Sebum
An oily secretion manufactured by tiny sebaceous glands that open into the hair follicles and that serves to keep the hair lubricated and shiny.
Theory of Donor Dominance
The scientific basis for hair transplantation stating that a hair’s genetic code resides within the hair follicle and not in the recipient site into which the hair is transplanted. The theory was first proposed by the Dermatologist Dr. Norman Orentreich in the 1950s. A Dermatologist was the first person/specialist to develop hair transplants.
Vasoconstrictor
A medication designed to constrict blood vessels. The most common one used in hair transplant surgery is epinephrine. It is added to the local anesthetic in hair restoration procedures to increase the duration of the anesthetic and to control bleeding.
Vellus Hair
Fine, peach-fuzz hair. It lacks a central medulla which is present in thick terminal hairs. In contrast to miniaturized hairs, which have varying diameters, vellus hairs are more uniform in size.
Vertex (Crown)
The region of the scalp posterior to the vertex transition point where the hair takes on a whorl pattern.
Vertex Transition Point (VTP)
The vertex transition point is the part of the back of the scalp where the horizontal and vertical planes meet. It lies just behind the highest part of the skull. It is the approximate point where the hair changes direction from a predominantly forward direction to a whorl. The VTP is important in that it represents a natural stopping point for a hair transplant when the donor hair reserves are limited.